
Oh, this is Chandra’s. The wheel of risk adjustment – that’s what I call it, not her.
Coach Chandra: I like that. It makes me think of a pizza.
Coach Alicia: Yeah!
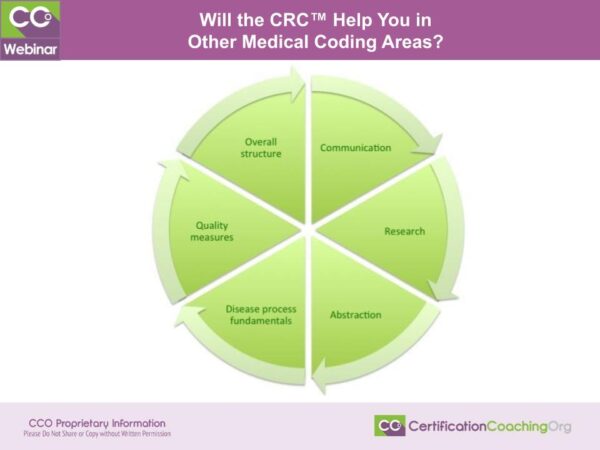
Coach Chandra: So the question we got here is, will the CRC® help you in other medical coding areas? This is an absolute great big bold print exclamation point YES! The skills that you need to pass the certification exam for the CRC and to really be successful in the risk adjustment arena are going to parlay into a lot of other areas.
So, communication. I’m going to start with communication. Communication is key across the board. Being able to communicate well both verbally as well as written is essential in healthcare. If you are not able to do that, (A) you’re going to tick a lot of people off. If you can’t, try to communicate the way you need to through written language and take a lot of things into consideration. I don’t know about you but if you’ve ever gotten that email that you just kind of interpret it incorrectly or you interpret it like, “Well, why would they say that?” We’ve got to be able to communicate. Much of our communication is done electronically and we’ve got to be able to do electronic communication, we’ve got to be able to support our point of view. We’ve got to be able to fact-check and do all of that. And that contributes across the board regardless of which area of healthcare you’re in, which certification exam you’re trying to pass. Good communication skills are essential.
 Research. I am a big, big, big advocate of research. A lot of that probably has to do with the fact that I worked for an attorney and I have an auditing background. That’s what I beat into my head. “Prove it.” Where does it say or what are you using to make the analysis that you’re making? So you’ve got to be able to research and prove your point, be able to link drugs and diseases together. And be inquisitive, be willing to learn. In addition to that, you’ve got to have strong abstraction skills. You’ve got to be able to read through a record and as Alicia said, be able to see that, “oh well, this patient is on hypertension and the provider refilled their lisinopril.” Well guess what, we dealt with that hypertension that day. Or they’re a diabetic and they’re on insulin and oh, their past, family and social history they had a pancreatectomy in 1999. Well, then we need to be clarifying are they a diabetic because they don’t have a pancreas anymore. Because the way we code that is a little bit different. There’s a lot of information that goes into abstraction. And the stronger your abstraction skills are, the more likely it is that you’re going to be able to find work in other areas like inpatient coding. Inpatient coding is predominantly abstraction and you’ve got to be able to read through those records and do the analysis and figure out what things are related and what aren’t in addition to inpatient coding. Clinical documentation improvement is all about being able to abstract and understanding the disease processes, pharmacology, pathophysiology – all of those pieces rolled together.
Research. I am a big, big, big advocate of research. A lot of that probably has to do with the fact that I worked for an attorney and I have an auditing background. That’s what I beat into my head. “Prove it.” Where does it say or what are you using to make the analysis that you’re making? So you’ve got to be able to research and prove your point, be able to link drugs and diseases together. And be inquisitive, be willing to learn. In addition to that, you’ve got to have strong abstraction skills. You’ve got to be able to read through a record and as Alicia said, be able to see that, “oh well, this patient is on hypertension and the provider refilled their lisinopril.” Well guess what, we dealt with that hypertension that day. Or they’re a diabetic and they’re on insulin and oh, their past, family and social history they had a pancreatectomy in 1999. Well, then we need to be clarifying are they a diabetic because they don’t have a pancreas anymore. Because the way we code that is a little bit different. There’s a lot of information that goes into abstraction. And the stronger your abstraction skills are, the more likely it is that you’re going to be able to find work in other areas like inpatient coding. Inpatient coding is predominantly abstraction and you’ve got to be able to read through those records and do the analysis and figure out what things are related and what aren’t in addition to inpatient coding. Clinical documentation improvement is all about being able to abstract and understanding the disease processes, pharmacology, pathophysiology – all of those pieces rolled together.
Disease process fundamentals. Understanding how a disease process works and how diagnoses are linked and what medications treat different conditions is going to make you stronger in any aspect of coding that you get into quite frankly. Because coding is all about translating medical record documentation to a code. It’s a foreign language or a translation for the most part. And the stronger that you are at understanding the disease process and the anatomy and pathophysiology, pharmacology, all of those aspects make you a stronger coder and you can begin to figure out, oh, well I wouldn’t have realized those two are related if I didn’t know about this disease process and if I hadn’t looked into this.
Quality measures. Now for purposes of risk adjustment, we talk predominantly about HEDIS and STAR. If you’re not familiar with HEDIS and STAR, you will be if you decide to take our course or if you sit for the CRC®. You have to learn about those. HEDIS is a national entity who sets quality measures. The purpose of their quality measures is to allow for comparability from plan to plan. Did you or did you not make sure the patient had a screening mammogram? Did you or did you not assess the patient’s body mass index? Those types of things. And those then parlay into the STAR measures for different health plans. They’re ranked on how well they did at those HEDIS measures in a number of other areas – customer service, quality of care, those types of things to get their STAR rating. And the STAR rating is just what we think about a star rating like if you book a hotel. Do you want a two-star hotel or a you want a five-star hotel? If you can afford it, you want the five-star. If you can get a really good deal on it, I want the best one that money can buy. Works the same way with the health plans. As a patient, I want the highest STAR rated plan I can afford or qualify for. And you find out not only how those quality measures work but then other quality measures begin to make sense like the Physician Quality Reporting System (PQRS) and Meaningful Use, the EHR initiative, the value-based modifier, and coming soon to a world near all of us, MACRA and MIPS. If you have no idea what MACRA and MIPS are and you’re planning on working in healthcare next year, go out and do a Google search. You’re going to find out that risk adjustment is coming to all plans in some way or another. Not just these Medicare Advantage Plans. MACRA and MIPS is requiring us to do more reporting on diagnosis codes and yes, it doesn’t affect physician payment until 2019. But that is based on 2017 claims data and we are rapidly approaching 2017.
As well as overall structure. If you understand the overall structure of risk adjustment, you kind of have a big picture of how healthcare in general works, how everything is interrelated, how physician claims drive so much more than just physician reimbursement. They drive health plan reimbursement, they drive hospital reimbursement. They drive all of these different pieces. So as you begin to accumulate skills, it’s very easy to extrapolate those to other areas in healthcare.
![[CCO] Certification Coaching Organization LLC [CCO] Certification Coaching Organization LLC](https://www.cco.us/wp-content/uploads/2015/05/CCO-Logo-2015-d3-500px.png)